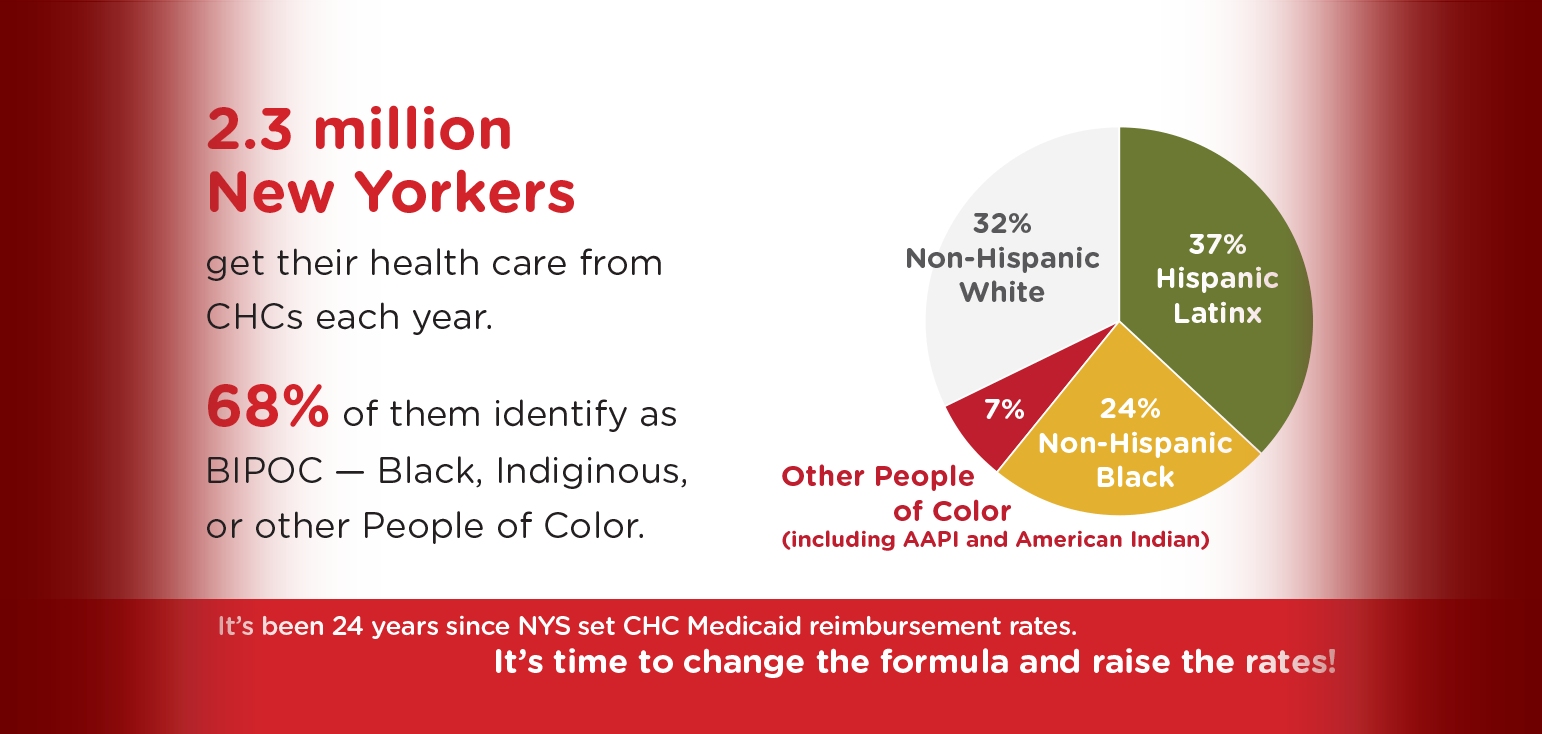
COMMUNITY HEALTH CENTERS ARE HERE FOR YOU.
Community Health Care Association is New York States voice for community-based primary care
Check out our new library
A useful tool on our new website, the improved library will let you sort, filter and search for resources in one place. Compiled by CHCANYS staff the library contains tools, materials, reference guides, video recordings and more from a variety of topic areas. From Digital Health and Clinical resources to Policy and Advocacy materials, find everything you need in one convenient database.